Cancer, the Emperor of All Maladies

After watching the recent Ken Burns documentary on PBS, Cancer, the Emperor of All Maladies, I felt the need to write about it, not so much because of its superb analysis of the history and state-of-the-art of allopathic cancer treatment, but because of what it left out.
I’m well acquainted with the limitations of allopathic cancer treatment, as I’ve described in my memoir, An Uncommon Cancer Journey, where clinical trials of the latest drugs did not heal my husband, Jack’s, esophageal cancer. But something else did — or a series of somethings else.
The kinds of alternative and complementary treatments we tried were completely left out of this six-hour PBS series, as were all the so-called “radical” discoveries made in this area during the time Jack and I were operating on a trial-and-error basis. At this same moment the nation was waging its “War on Cancer,” and big-time, big-money cancer research was, with considerable publicity, engaged in the same trial-and-error strategy.
Nonetheless, Ken Burns, documentarian par excellence, has given us a powerful story, tracing the history of cancer research from the time of the seventeenth century occupational physician Bernardino Ramazzini all the way to the stunning advances in molecular biology of the near-present. His film is based on the book Emperor of All Maladies: A Biography of Cancer, by Siddhartha Mukherjee, M.D., who also acts as an effective narrator in the film.
Children as Casualties

Again and again, I was struck by how much suffering was imposed by the medical profession in its quest, not only for an overall cancer cure, but for individual cures in individual cases. The military aspect of the “War on Cancer” became abundantly clear, and it seemed that so often the casualties were children. It was as if doctors and parents conspired to try anything, ANYTHING, to keep these children alive. In the early days they all died, many after treatments that were essentially torture. As the research progressed, some of them lived, although often for only a few additional months. After these kinds of heroic treatments was anyone able to die peacefully? If so, they weren’t given much footage in this film.
It’s true that there were some touching scenes of a sensitive young oncologist in West Virginia who counseled her patients that they did have a choice in whether or not to continue treatment. And she knew that “treatment” meant more suffering and probably an agonizing death.
Instead, they could go into hospice, where everything centered around comfort and making the patient’s remaining days more satisfying. I wondered why progress in cancer treatment needed to entail so much suffering.
The Cycle of Hope and Disappointment
The film’s commentators repeatedly alluded to the cycle of great hope and crushing disappointment as each new breakthrough proved to be a failure — as each oncogene proved to be resistant to the therapy that had been so painstakingly and expensively developed to conquer it, and each new targeted immunotherapy was found to be effective only in limited cases.
Each time a little girl with a rare kind of leukemia was cured, other little girls died because the treatment just didn’t work on them.
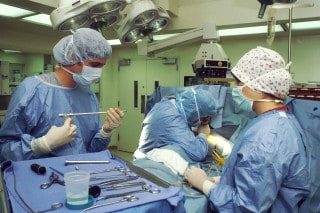
After a while I got the feeling that the whole six-hour series was a story of obsession — a community of driven scientists partnered with drug manufacturers experimenting on near terminal subjects who had been given the tantalizing hope of a cure. Sometimes if one drug wasn’t enough, they would try two, or three, or four, and patients would endure excruciating effects in a desperate attempt to become well again, usually to no avail.
Prevention

There was some discussion in the film about prevention as a more viable solution. Prevention was given credit for the recent reduction in cancer rates, at least in the U.S., resulting from early detection, smoking cessation, and certain targeted therapies, particularly for cervical cancer, some melanomas, and kidney cancer.
In the end, the program concludes that it is unlikely that any single treatment or even all of them working together will ever eliminate cancer completely. The author, Dr. Mukherjee acknowledges that cancer cells are evolving to resist the therapies developed to treat them, but maintains that we are also evolving with new drugs, new research, and possible new breakthroughs. I’m not convinced that this painful and expensive race will ever be won, or even if it is a good idea to pour billions of dollars into drug research only to stay a few paces ahead of the mutations.
Alternatives
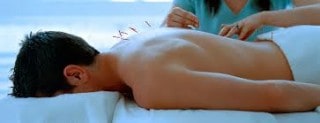
In the mean time, what about all the treatments that were left out of this agonizing cycle of hope and despair? The Ken Burns series made no mention of a host of non-drug alternatives that could at least help patients to be more comfortable, and possibly contribute importantly to their healing. Many of the mainstream cancer treatment centers have now added treatments like acupuncture, psychotherapy, nutrition, meditation, yoga, exercise, and other helpful programs, probably due to public demand. However, none of these was addressed in the film.
Neither was the ever increasing body of research supporting the healthful, even curative properties of these treatments. In fact, most of the allopathic community wouldn’t even consider them treatments.
Candace Pert: Courageous Pioneer

There was no mention of the groundbreaking discoveries of scientists like Candace Pert and others who were pushing the psychoneuroimmunology envelope. Around the time that Jack Hardesty received his “terminal” diagnosis from the National Cancer Institute, Candace Pert, Ph.D. was chief of the Section on Brain Biochemistry, Clinical Neuroscience Branch, of the National Institute of Mental Health, both under the umbrella of the National Institutes of Health (NIH). Jack and I had actually heard of her work while we were living in the area. Although we knew that she was a research pioneer, we really had no idea at that time of the importance of her discoveries.
As a young graduate student in 1972, Candace Pert discovered the brain’s opiate receptor, and later went on to elucidate the role of neuropeptides in emotion and immunity, hence the title of her book, Molecules of Emotion: The Science Behind Mind-Body. She is credited with launching the field of molecular neuropharmacology and popularized the term “Bodymind.” She proved that the “mind” is not only in the head, as we usually assume, but is located throughout the entire body and that there is constant communication between cells everywhere and the central nervous system.
In one of her scholarly papers Dr. Pert states: Neuropeptides and their receptors thus join the brain, glands, and immune system in a network of communication between brain and body, probably representing the biochemical substrate of emotion.
Life was not always easy for Candace Pert, a brilliant woman in a sea of ambitious male researchers. When she was passed over for an especially prestigious award, with her male counterparts receiving the credit that was due her, she was not quiet about criticizing the establishment, and eventually left her position at the NIH.
The Glories of War

In Molecules of Emotion Dr. Pert draws attention to the militaristic party line, quoting an article in Parade magazine entitled “What Medicine Will Conquer Next.” Fourteen leading biomedical researchers, some of them Nobel Prize winners, responded in what she calls, “a paean to the glories of high-tech, high-cost modern medicine, with particularly glowing praise heaped on genetic research as the answer to all our ills.” The exception to this accolade occurs at the end of the article, where Dr. Bernadine Healy, former director of the NIH states: “Changing your lifestyle can make a difference.”
Bodymind and the Immune System
Dr. Pert had noticed the research of a contemporary, Dr. J.E. Blalock, demonstrating the interconnectedness, or “oneness” of the body and mind, which, even in 1984 was referred to as the “brainbody connection,” precursor of the term, “Bodymind.” Blalock had published his research showing not only that the brain affects the immune system, for which there already was grudging acceptance, but that the effect is reciprocal. The immune system also affects the brain, secreting lymphocytes and peptides like endorphins. This process produces physiological and even behavioral changes in the diseased animal (or human).
Dr. Blalock’s 1984 article, The Immune System as a Sensory Organ caused a furor among research scientists at the time. In response, Dr. John Maddox, then editor of the prestigious journal Nature, referred to scientists like Blalock and Pert as “radical psychoimmunologists,” a title they most likely bore proudly.
A year later, Blalock pointed out in his article, The Immune System: Our Mobile Brain? that his work had been replicated by other scientists several times over. Although Dr. Blalock has remained firmly rooted in the scientific community, he published a comprehensive review in 2005 with the intriguing title The Immune System as Our Sixth Sense.
Many well known medical professionals have supported these findings, and many more studies have taken place since then. These names include physician/authors such as Larry Dossy, Bernie Siegel, Christianne Northrup, Dean Ornish, Andrew Weil, and more. And yet, medical schools and most practicing physicians still employ the old Cartesian split between body and mind, considering the body a physical machine.
Biology of Belief

Author and biomedical researcher Bruce Lipton, Ph.D. has studied these phenomena starting with the operations of single cells and progressing to the point where, like Candace Pert, he concludes that communication between the community of cells in every system can be considered one bodybrain.
In his book The Biology of Belief, Dr. Lipton points to the placebo effect, which he calls the “Belief Effect” as a testament to body mind, an example of a place where all of medicine can agree, but one that is skipped over lightly by most of the allopathic community. He also mentions the negative consequences of the “nocebo” effect, epitomized by the all too common admonition, “You have six months to live.”
Nine Key Factors
Another source of inspiration in non-medical healing is the book Radical Remission, recently published by Kelly Turner, Ph.D. Dr. Turner, a psychotherapist trained as an oncology social worker, explores the cases of several cancer patients who became well, defying the odds of serious or terminal cancer prognoses.
Dr. Turner arrives at nine key factors that she found in nearly every one of her subjects. These include diet and supplements, as one might expect, but importantly they also include other less tangible factors: taking control of your health, following your intuition, embracing social supports, releasing suppressed emotions, increasing positive emotions, deepening your spiritual connection, and having strong reasons for living. It seems that these key factors are very consistent with the findings of Pert, Blalock, and Lipton — all related to the concept of bodymind.
Jack Hardesty’s Bodymind
When I reflect on my husband’s “miraculous” healing, it all makes perfect sense. Jack never disparaged his allopathic treatment as part of the clinical trial at the National Cancer Institute, or later his treatment at the Janker Klinik in Bonn. Despite the fact that the doctors were unable to cure his cancer, they bought him time, and his activities during that extra time were undoubtedly critical to his healing.
With the help of an exceptional therapist, Jack released decades worth of repressed anger and grief, he quit his hated job and found work that he enjoyed, he stopped drinking, he healed his marriage, and he followed his dream of opening an art gallery. All of this without the benefit of designer drugs because the Designer of his bodymind already knew how to do it.






11 thoughts on “Bringing Peace to the War on Cancer”
Great Blog Alice! Yes, Amen. I have discovered as I age that I’m less afraid of
death and more afraid of the torture of treatment regiments and fear induced by
the medical community. I recently went to a doctor to be sure I was being “followed”
for one condition and was told I was likely at risk for another. I’m tired of going in
healthy and being scared sick.
Karen
Karen – Just get those little peptides moving and enjoy doing what you love to do! Let’s hear it for placebo rather than nocebo.
Thank you for this interesting and terrific article, Alice!
Love the title. Love the content. Love the author. 🙂
Another great invitation Alice, to those that would like to treat the whole person and not just the disease.
Thanks, Angela. I think the medical community is beginning to wake up to the concept of the whole person. But big pharma, not yet.
Thanks for balancing the scales a bit! Reductionist, high-tech medicine seems a well-oiled system with far too much money and too many egos at stake to accept other (less expensive and profit-making) solutions appear to exist. But it needs to be challenged so people can make informed choices how they will address cancer if it strikes them.
Choices, for sure! And unless you know about the availability of options, you’re not going to be able to make informed choices. I’m not denying the progress that’s been made in chemotherapy and surgery, especially with early detection, but there’s so much more.
Dear Alice,
You are doing such good work to help us know how to think about the care of our mindbodies. We are looking forward to our conversations when you visit us in May.
Alice, thank you for your erudite review of the parallel movement (along with the ‘war on cancer’) that is replacing the materialistic cosmology of today’s science. Candace’s ‘bodymind’ worldview helped birth a mindset that says all aspects of the universe are intertwined and powered by a primal consciousness. Its obvious that its energy is designed to stimulate and evolve intelligent beings who become capable of creating themselves. Learning how to use our mind to keep one’s physical health intact is one of our primary objectives. Only then can we manifest our abilities to become multidimensional beings.
It amazes me how blind we are to the truth you have shared. Many people would rather suffer the poisoning of chemotherapy that do the work of having a healthier lifestyle. Personally, I don’t get it.
Thanks for your comment. Personally, I wouldn’t necessarily refuse chemotherapy, but I would certainly chose every lifestyle change at the same time, or even before, especially cancer counseling.